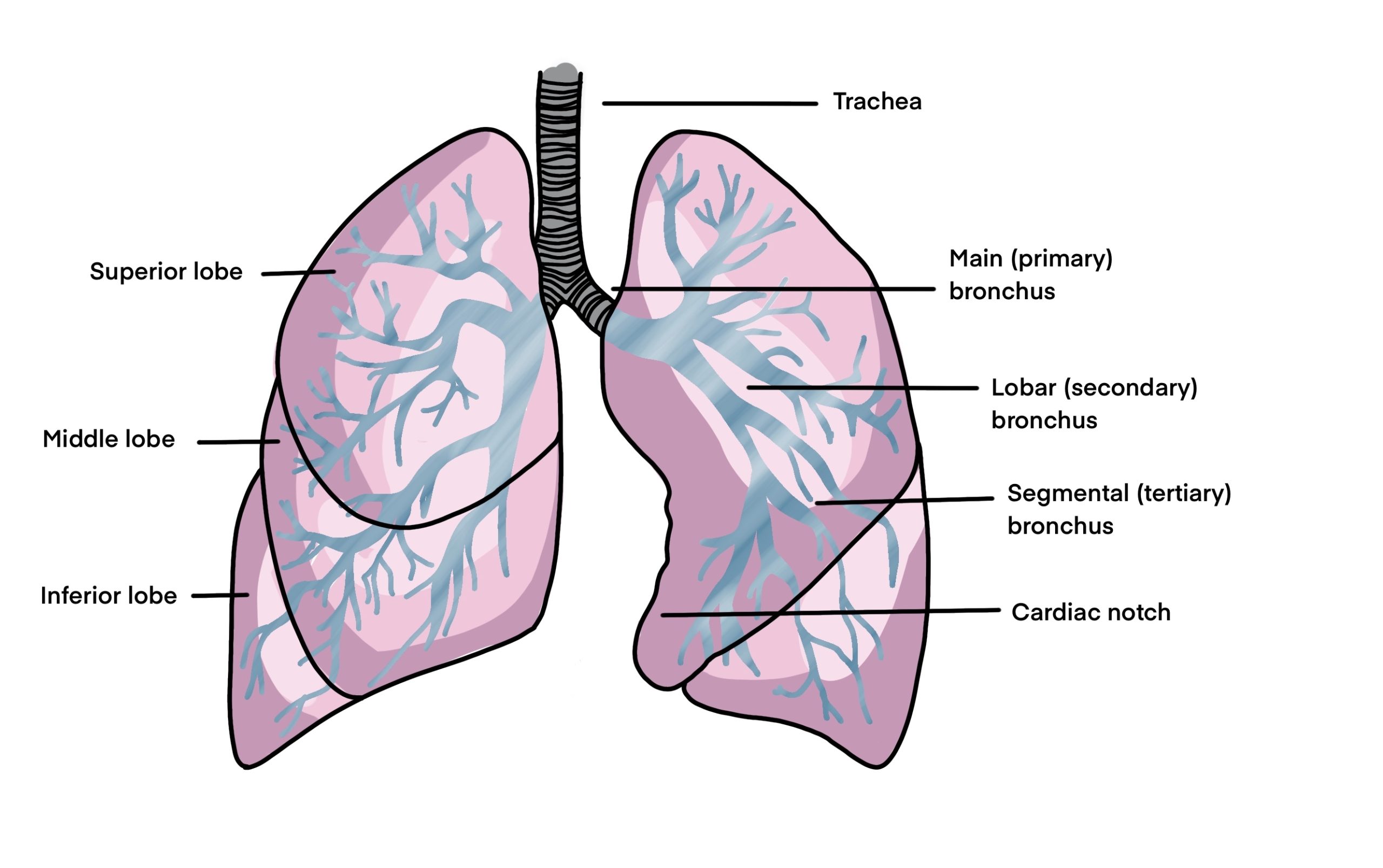
According to a study published in The New England Journal of Medicine, recent improvements in the detection of small-sized peripheral non-small-cell lung cancer (NSCLC) have renewed consideration of sublobar resection in place of lobectomy in patients with NSCLC.
Based on the trial’s data, the lead author, Nasser Altorki, reported that sublobar resection was not inferior to lobectomy in terms of disease-free survival among patients with peripheral NSCLC with tumors of 2 cm and without hilar and mediastinal lymph node positivity. Overall survival was reportedly similar between the two procedures as well.
Sublobar Resection Comparable With Lobectomy in NSCLC
This was a multicenter, noninferiority, phase 3 trial that enrolled 697 patients with NSCLC clinically staged at T1aN0 (tumor size, ≤2 cm) from June 2007 to March 2017. Of the participants, 340 underwent sublobar resection and 357 underwent lobar resection, respectively, after intraoperative confirmation of node-negative disease status.
The primary end point of the trial was disease-free survival, defined as time from randomization until disease recurrence or death from any cause. Key secondary end points included overall survival, locoregional and systemic recurrence, and pulmonary functioning.
Researchers found that sublobar resection was noninferior to lobar resection for disease-free survival (hazard ratio [HR], 1.01; 90% CI, 0.83-1.24) over a median follow-up of 7 years. Likewise, overall survival was comparable between the two procedure groups (HR, 0.95; 95% CI, 0.72-1.26).
In addition, the 5-year rate of disease-free survival was 63.6% (95% CI, 57.9-82.9) in the sublobar resection group compared with 64.1% (95% CI, 58.5-69.0) in the lobar resection group. The 5-year rates of overall survival were also similar at 80.3% (95% CI; 75.5-84.3) and 78.9% (95% CI; 74.1-82.9) after sublobar and lobar resection, respectively.
Lastly, the authors observed no significant differences in terms of locoregional or distant recurrence and, at 6 months post-procedure, there was a between group difference of 2% in median percentage of predicted forced expiratory volume in 1 second, favoring the sublobar resection group.
“In patients with peripheral NSCLC with a tumor size of 2 cm or less and pathologically confirmed node-negative disease in the hilar and mediastinal lymph nodes, sublobar resection was not inferior to lobectomy with respect to disease-free survival,” Altorki and colleagues summarized.






 © 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.
© 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.